Peritoneal Dialysis | Vibepedia
Peritoneal dialysis (PD) is a critical medical treatment for kidney failure, employing the patient's own peritoneum—the membrane lining the abdominal…
Contents
Overview
Peritoneal dialysis (PD) is a critical medical treatment for kidney failure, employing the patient's own peritoneum—the membrane lining the abdominal cavity—as a natural filter. This method facilitates the exchange of fluids and waste products directly from the bloodstream, offering a less invasive alternative to hemodialysis. PD provides greater flexibility in treatment schedules, allowing many patients to manage their therapy at home, thereby enhancing quality of life and enabling greater autonomy. While it boasts superior outcomes in the initial years of treatment and better tolerability for individuals with cardiovascular conditions, its efficacy hinges on meticulous technique and patient adherence. As a cornerstone of renal replacement therapy, PD continues to evolve with technological advancements, aiming to improve patient outcomes and accessibility worldwide.
🎵 Origins & History
The concept of using the peritoneal membrane for dialysis emerged in the early 20th century. Georg Ganter successfully removed excess fluid from patients using a sterile solution introduced into the peritoneal cavity. The development of specialized dialysis solutions and the refinement of sterile techniques by researchers at institutions like the University of Pittsburgh in the subsequent decades solidified PD's place as an essential medical intervention, recognized by its inclusion on the World Health Organization's List of Essential Medicines.
⚙️ How It Works
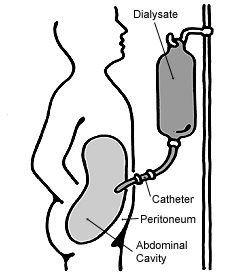
Peritoneal dialysis operates on the principle of diffusion and osmosis across the peritoneal membrane. A sterile dialysis solution, typically containing dextrose, is infused into the peritoneal cavity via a surgically implanted catheter. The high concentration of dextrose in the solution draws excess fluid and waste products, such as urea and creatinine, from the blood vessels within the peritoneum into the cavity. This exchange, known as an 'exchange,' typically lasts for several hours. After the dwell time, the used solution, now containing the removed toxins and excess fluid, is drained from the abdomen. This process is repeated multiple times a day for continuous ambulatory peritoneal dialysis (CAPD) or automated peritoneal dialysis (APD) overnight, effectively mimicking the kidney's filtering function.
📊 Key Facts & Numbers
Globally, an estimated 10% of all dialysis patients, numbering over 3 million worldwide, utilize peritoneal dialysis. In 2023, the global PD market was valued at approximately $5.5 billion, with projections indicating a compound annual growth rate (CAGR) of 6.2% through 2030. Approximately 50% of PD patients worldwide are in Asia, with significant adoption rates in countries like China and India. In the United States, PD accounts for roughly 8% of all dialysis treatments, representing over 40,000 patients. The average cost of PD treatment per patient per year is estimated to be between $40,000 and $60,000, often proving more cost-effective than hemodialysis over the long term, especially when considering home-based care.
👥 Key People & Organizations
While Georg Ganter pioneered early concepts, key organizations like the International Society for Peritoneal Dialysis (ISPD) play a crucial role in advancing research, setting clinical guidelines, and fostering global collaboration among nephrologists and researchers. Companies such as Baxter International and Fresenius Medical Care are major manufacturers of PD solutions and equipment, driving innovation in delivery systems and catheter technology. The National Kidney Foundation in the US and similar bodies worldwide advocate for patient access and education regarding PD options.
🌍 Cultural Impact & Influence
Peritoneal dialysis has profoundly influenced the lives of millions by offering a degree of freedom and normalcy previously unattainable with traditional dialysis. The ability to perform treatments at home, often during sleep, allows patients to maintain employment, pursue education, and engage in social activities with fewer disruptions. This autonomy is a significant cultural shift, empowering individuals to manage their health proactively. PD has also fostered a strong sense of community among patients, with online forums and support groups providing vital peer-to-peer connection and shared experiences. The visual representation of PD, often involving a discreet catheter and dialysis bags, has become a recognizable symbol of resilience and adaptation in the face of chronic illness.
⚡ Current State & Latest Developments
The landscape of peritoneal dialysis is currently marked by continuous innovation in automated peritoneal dialysis (APD) systems, which offer enhanced patient convenience and improved fluid management. Wearable and miniaturized PD devices are under development, aiming to further reduce the burden of treatment and improve patient mobility. Telehealth and remote monitoring technologies are increasingly integrated into PD care, allowing healthcare providers to track patient adherence and vital signs more effectively, thereby enabling earlier intervention for potential complications. Furthermore, research into novel dialysis solutions with improved biocompatibility and reduced osmotic stress is ongoing, seeking to enhance the long-term health of the peritoneal membrane.
🤔 Controversies & Debates
A significant controversy surrounding PD revolves around the risk of peritonitis, an infection of the peritoneal membrane, which can lead to treatment failure and necessitate a switch to hemodialysis. Patient adherence to strict sterile techniques is paramount, and variations in patient education and socioeconomic factors can influence infection rates. Another debate centers on the long-term viability of the peritoneal membrane itself; while generally robust, it can degrade over time, leading to reduced efficacy. The cost-effectiveness of PD versus hemodialysis is also a subject of ongoing discussion, with varying healthcare system reimbursement models influencing physician and patient choices.
🔮 Future Outlook & Predictions
The future of peritoneal dialysis is poised for significant advancements, driven by the pursuit of greater patient independence and improved long-term outcomes. Next-generation APD machines are expected to feature enhanced artificial intelligence for personalized treatment optimization and predictive analytics to anticipate complications. The development of bio-compatible membranes and solutions that preserve peritoneal function for longer durations is a key research focus. Furthermore, the integration of nanotechnology in dialysis solutions could offer novel ways to remove toxins more efficiently. Experts predict that PD will become an even more prominent treatment modality, particularly in low- and middle-income countries, due to its potential for home-based care and lower infrastructure requirements compared to hemodialysis centers.
💡 Practical Applications
Peritoneal dialysis is primarily applied as a life-sustaining treatment for individuals suffering from end-stage renal disease (ESRD) when their kidneys can no longer adequately filter waste products and excess fluid from the blood. It is particularly beneficial for patients who are not suitable candidates for hemodialysis due to cardiovascular instability, or those who prefer the flexibility of home-based treatment. PD is also utilized in acute settings for patients requiring rapid fluid removal or correction of electrolyte imbalances. The practical application involves patient training in sterile techniques, catheter care, and the management of dialysis exchanges, often facilitated by specialized PD nurses and home care support teams.
Key Facts
- Category
- science
- Type
- technology